WHAT IS GYNECOMASTIA | CHICAGO, IL
What is Gynecomastia?
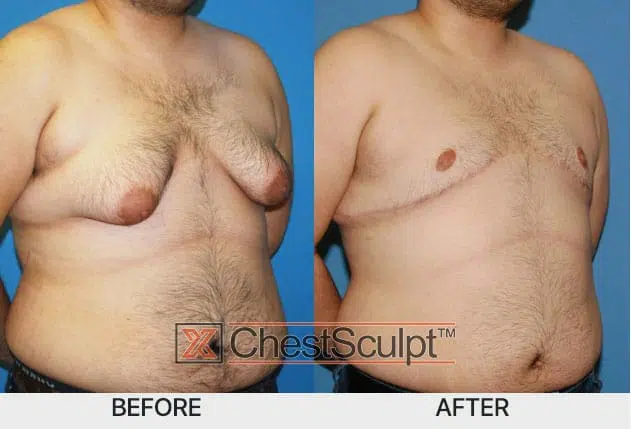
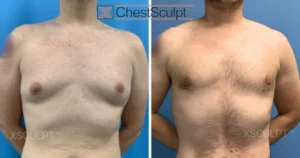
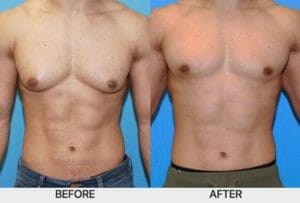
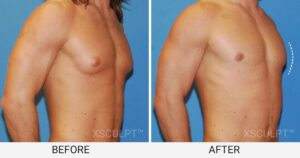
The female appearance of breasts in males is called “gynecomastia”. It commonly occurs during adolescence due to hormonal changes during puberty. Although it is a physical disease, it is the emotional feelings of embarrassment and lack of self confidence that is the devastating part of this problem.
During adolescence, it can reduce in size at the end of puberty generally requiring no treatment. However, if it continues into adult life it is mostly likely permanent and can lead to low self-esteem and a lack of confidence. Surgery then becomes the only option to solve the problem.
WHAT IS GYNECOMASTIA | CHICAGO, IL
What is Gynecomastia?
The female appearance of breasts in males is called “gynecomastia”. It commonly occurs during adolescence due to hormonal changes during puberty. Although it is a physical disease, it is the emotional feelings of embarrassment and lack of self confidence that is the devastating part of this problem.
During adolescence, it can reduce in size at the end of puberty generally requiring no treatment. However, if it continues into adult life it is mostly likely permanent and can lead to low self-esteem and a lack of confidence. Surgery then becomes the only option to solve the problem.
GYNECOMASTIA: WHAT IS IT?
Gynecomastia is derived from the Greek words gynec meaning feminine and mastos that means breasts. Literally, the term “male breast” is relative to a condition that results in excessive growth and enlargement of breast tissue in men.
The male breast consists of both glandular tissue which is composed of ductal and stromal elements, as well as adipocytes or “fatty tissue”. The excessive growth of glandular tissue results in overgrown breasts in males that are unsightly and embarrassing for men. Patients with severe gynecomastia may have excess skin leading to considerable ptosis (or sagging) of the breast.
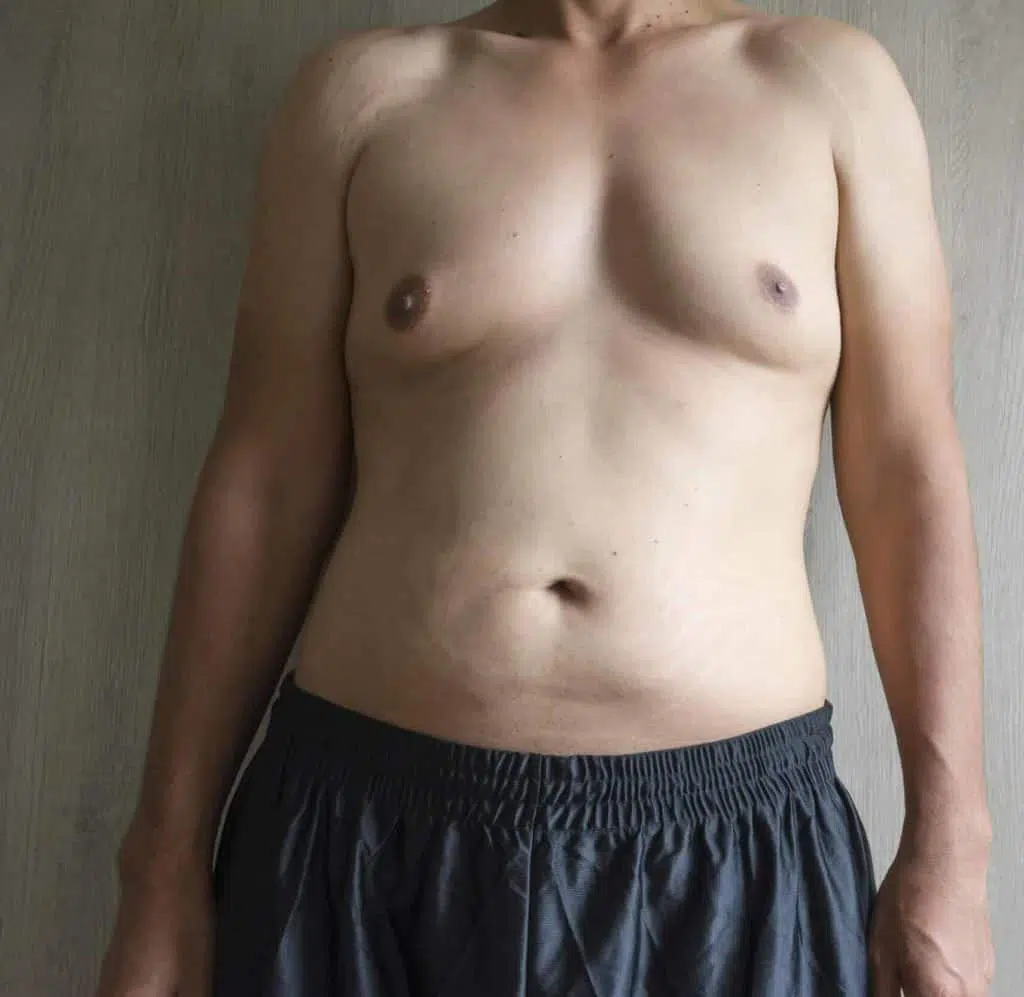
CHANGES ARE SEEN AT A CELLULAR LEVEL
Gynecomastia is derived from the Greek words gynec meaning feminine and mastos that means breasts. Literally, the term “male breast” is relative to a condition that results in excessive growth and enlargement of breast tissue in men.
The male breast consists of both glandular tissue which is composed of ductal and stromal elements, as well as adipocytes or “fatty tissue”. The excessive growth of glandular tissue results in overgrown breasts in males that are unsightly and embarrassing for men. Patients with severe gynecomastia may have excess skin leading to considerable ptosis (or sagging) of the breast.
PATHOPHYSIOLOGY
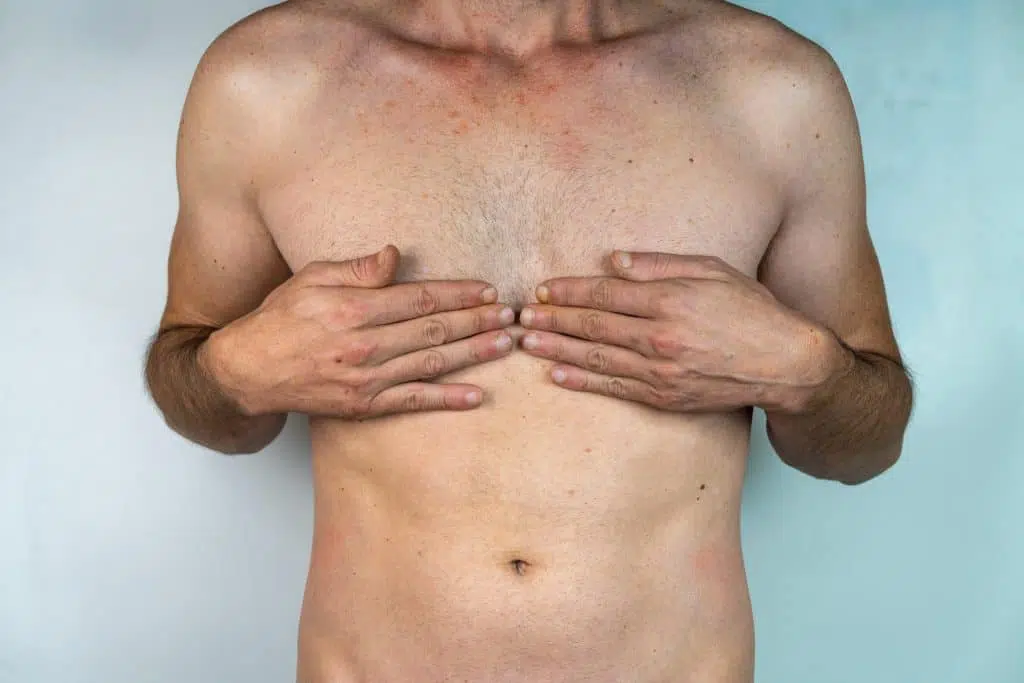
95% of free circulating testosterone is secreted by the testicles. The testicles are also responsible for 15% of estradiol as well as 5% of estrone on a daily basis. These two compounds are responsible for the estrogenic effects in the body.
80% of the estrogen in males is produced by the conversion of testosterone, with the help of the enzyme aromatase. This enzyme acts on breast and subcutaneous fat, liver, skin, kidneys as well as on your muscles by converting testosterone into estrogen. Both age and higher levels of body fat percentage are responsible for enhanced activity of the aromatase enzyme because the enzyme is found mainly in fat cells.
The testosterone to estrogen ratio can get imbalanced in the following conditions:
- Adrenal glands or the testicles secreting too much estrogen into the blood
On the other hand, the imbalance can also be due to the following reasons:
Studies have been done that suggested exposure to certain substances in the environment that have weak estrogen effects can induce the condition of gynecomastia. Air pollutants, radiations, organochlorine pesticides, fuels, and plasticizers are some of those chemicals that are known to cause gynecomastia.
There are other hormones aside from estrogen that may cause gynecomastia. The male breast contains receptors of luteinizing hormone as well as human chorionic gonadotropin hormone. Activation of these receptors can decrease the protective testosterone effect on breast tissue. Another hormone, progesterone, acts with insulin growth factor-1 to cause proliferation of the glands of the breast. Increase in progesterone in males can be seen in conditions such as hyperthyroidism and in liver cirrhosis. Therefore, in patients with these conditions plus gynecomastia it is important to test their progesterone levels.
SIGNS AND SYMPTOMS
Although not a deadly condition, gynecomastia can be difficult to deal with especially if it is also accompanied by pain. The major symptom of gynecomastia is swelling of the male breast tissue. This swelling is the proliferation of the breast gland tissue rather than the fat tissue itself. The breast gland often has a firm or rubbery texture.
Gynecomastia commonly occurs on both sides but in some cases can also be one-sided. Even if it occurs bilaterally, it isn’t uncommon for one side to be larger than the other.. If pain does occur, it is usually mild with some tenderness and sensitivity.
It is important to differentiate gynecomastia from male breast cancer. Cancer generally involves one side, not necessarily centered surrounding the nipple, and can be associated with skin dimpling, nipple inversion, and nipple discharge. Advanced cases may have enlargement of the lymph nodes of the underarms.
GYNECOMASTIA: COMMON CAUSES
Hormonal Changes
Gynecomastia is caused mainly by a greater reduction in the protective effects of testosterone, as compared to estrogen. This can occur due to blockage of testosterone effects, decreased testosterone levels, or an increase in estrogen levels.
Although estrogen and testosterone are mainly female and male hormones, both hormones are present in both sexes. Estrogen is more in quantity in females and testosterone in males. When the hormones become imbalanced and higher levels of estrogen are present in males as compared to testosterone, the result will be conditions such as gynecomastia.
Medications
Breast enlargement due to hormones can affect males as infants (because of mother’s estrogen), during puberty when the hormonal levels can be imbalanced, and in adulthood at the age of 50 to 69 often as side effects of certain medicines. Medications that can cause gynecomastia includes:
- Steroids and androgens
Supplements
Physiological or non-physiological ailments
- Hypogonadism: Normal testosterone production is disturbed, e.g. Klinefelter syndrome, pituitary insufficiency
- Aging: The process of aging involves hormonal changes, usually decreasing testosterone, that can cause gynecomastia, particularly in overweight men.
- Tumors: Tumors involving glands that are involved in hormone production such as the testicles, adrenal glands, or pituitary gland can alter the hormone balance.
- Hyperthyroidism. high levels of the hormone thyroxine can lead to gynecomastia
- Kidney failure and dialysis. Patients undergoing dialysis experience gynecomastia due to the dysfunction of Leydig cells of the testicles causing low testosterone.
- Liver failure. Medications for liver disease can produce hormonal imbalance causing gynecomastia. Cirrhosis can cause increased estrogen levels leading to gynecomastia development.
- Malnutrition. Gynecomastia can occur due to a drop in testosterone when your body is not getting enough nutrition while estrogen levels are unaffected. Breast enlargement can also occur when malnutrition is reversed due to the resulting hormone imbalance.
- Aromatase excess syndrome. This is due to a congenital defect, which results in excessive production of estrogen. This condition not only leads to gynecomastia, but also several other physical manifestations such as reduced height due to premature epiphyseal fusion of bones.
DIAGNOSIS
- One-sided
GYNECOMASTIA: RISK FACTORS
Complications
MANAGEMENT OF GYNECOMASTIA
Medical treatment is attempted if gynecomastia
There are 3 categories of medical treatment for gynecomastia:
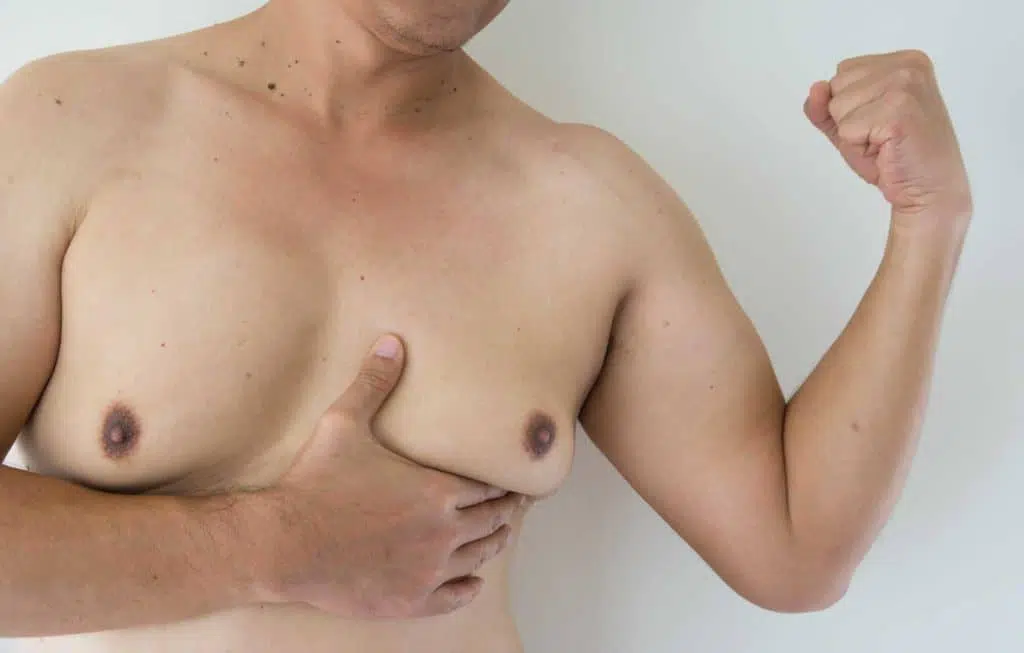
How to Prevent Gynecomastia
There are 3 categories of medical treatment for gynecomastia:
GRADES OF GYNECOMASTIA
GYNECOMASTIA SURGERY
Surgical intervention would be recommended if:
Surgical Techniques